How Diabetes Changed My Life
Photo courtesy of the Hanlon family
Abby Hanlon is learning to live with Type 1 Diabetes, a disorder that prevents her body from making insulin.
December 9, 2020
It was a lovely late-summer morning, and I was ready for a full day of work ahead of me. Little did I know, I’d end up rushed to the hospital hours later.
With a history of Type 1 Diabetes running in my family, the disease was always something in the back of my mind. I knew the signs to look out for, but I never took it very seriously; I never considered it a real possibility.
I had grown up watching my aunt insert insulin into her body under the dining table before a holiday meal, and had once witnessed a lady question my cousin if she was doing drugs at a restaurant. As curious as I was about the whole injection process, I never really thought it was my place to ask.
All of that changed when I noticed I had been drinking a lot more water than usual– and when I say a lot of water, I mean a lot of water. Seven to eight glasses per meal was becoming a normal habit of mine, and with drinking a lot of liquids came an abundance of bathroom breaks. On the way up to my friend’s lake house, I found myself frequently asking to stop, making the 5-hour road trip that much longer. For the duration of my time up in Wisconsin, I felt groggy, irritable, and extremely low-energy; if you know me, you’d notice I wasn’t acting like myself.
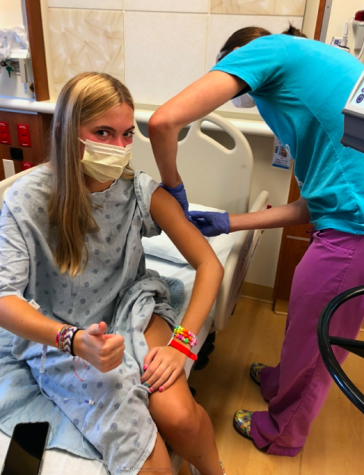
Just a week later, I went in for my annual school physical. I brought up my symptoms and my concern for possibly developing diabetes. The nurse lightheartedly joked that I was probably just dehydrated and didn’t think I had it, but continued to run a test of my blood sugar anyway. Minutes later, the visit took a turn. My distressed pediatrician rushed through the door: “You need to go to the ER now.”
Upon arrival at Lurie’s Children’s Hospital in Chicago, I was overwhelmed with an abundance of friendly nurses, doctors, and the recurring theme of ocean and wildlife within each hospital floor. I was quickly forced to get over my fear of IVs, as one was quickly pushed into my arm the minute I tucked myself under the hospital blankets. The next few hours were filled with injections, finger pricks, calculations, tears, and a boatload of questions.
According to the doctors, blood sugar for children at my age and health should range between 80 and 150 units. Mine was at 500.
My body wasn’t generating insulin, a hormone produced in the pancreas which controls the amount of glucose, or sugar, in the blood. This hormone is essential because its sole purpose is to preserve nutrients from food and liquids that keep you energized throughout the day. Although my body had once produced insulin, the production of the hormone was halted once my blood cells began to attack my pancreas.
For lack of better words, I had been energizing my body through plenty of food and liquids, but none of which was being used due to my shortage of insulin.
I was doing all that I could, yet I wasn’t receiving anything in return.
This information may seem overwhelming and hard to understand; trust me, I felt the same way. Within a day and a half in the hospital, I was forced to learn how to count carbohydrates in my meals, calculate the right dose of insulin, and inject it into my body. I was angry, deeply confused, and absolutely exhausted.
Injecting needles into your body is truly the strangest, and scariest feeling. It wasn’t until my first meal outside of the hospital that I realized this is my new reality. My cheeseburger in front of me wasn’t just a cheeseburger anymore, it was the number of carbs in the bun, plus the toppings, and the side. My questions weren’t so focused on how my parents’ meals were, they were “How many units of insulin do I inject into myself?” and “Am I even doing this right?”
My anxieties about social situations began to increase. I didn’t want to stand out every time I got food with friends or went to a social event. I didn’t want people to think “that’s the girl with diabetes” every time they saw me. It can be frightening to be different with something so new and life changing.
However, I quickly experienced kindness in the new community I became apart of. Even as the struggle continues to endure, I know I have a countless supply of support and assistance — and that truly makes all the difference.
My friends and family have been extremely patient and flexible based on my needs and concerns. As hard as it is for me personally, it can also be challenging for those closest to me as well. They have been very understanding, from checking in on me and my blood sugar numbers to providing me information about other families and teenagers with similar situations. I have become very connected with the teenage diabetes community and have loved every second of it.
While in the hospital, one of my doctors explained, “Diabetes is a love-hate relationship. You’re going to have days where you feel like you can do anything, and others where all you want to do is cry about it.” Although there have been some ups and downs, every day is a learning experience that I, myself am truly grateful for. I’ve learned that having diabetes doesn’t define me, it only makes me stronger.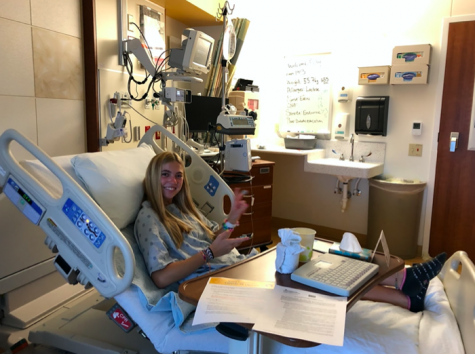








Mike MacDougal • Dec 11, 2020 at 2:56 pm
Well done Abby!! This is a great article and your conclusions are spot on. You are an impressive girl to attack this change head on so well. I’m sure you will inspire and help others by example.
Robert Parry LFHS Staff • Dec 11, 2020 at 8:57 am
Great article Abby!
My wife is T1 also, and reading the article reminded me of her diagnosis as she went through all those same feelings.
Hang in there, lean on your family and friends in the tough moments, and be brave and inspirational to others when you are able!!-rp
Buffy Stauffer • Dec 9, 2020 at 4:00 pm
So beautifully written, Abby! I know you will inspire everyone you meet by being so brave and so honest.
Jacob • Dec 9, 2020 at 10:28 am
WOW!!! Great article, Abby!! People like you and I with T1D can be an inspiration to younger kids with Type 1 Diabetes! Also, btw, you are a talented writer!!! I love this!! ? ??
Sophie Huddlestun • Dec 9, 2020 at 10:01 am
Abby- you’re incredible, as always. So proud of you for not losing your smile during this crazy year. Thanks for being you!
Tegan Heswall • Dec 9, 2020 at 9:45 am
Abby,
Thank you for being so brave and writing about your story. ♥️
Jennifer Mower • Dec 8, 2020 at 8:18 pm
Abby
You are amazing! This is beautifully written. Mowers are behind you all the way. Sending love and support
Ciara Frost • Dec 8, 2020 at 5:56 pm
Abby,
This article is brave and beautifully written. Thank you for sharing your experience. You are an inspiration to us all I look forward to watching you continue to thrive, despite this challenge. ????